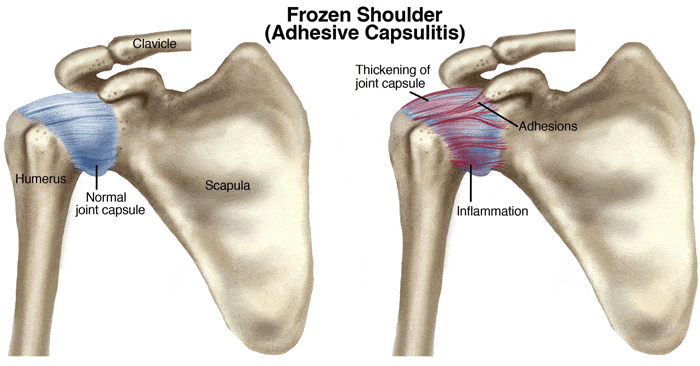
What is Frozen Shoulder (Adhesive Capsulitis)?
Like many professions out there, medicine has its own language. In order to become fluent in medicine, one needs to become familiar with an abundance of acronyms, abbreviations, endless eponyms, complex medical terminology, and even Latin. All of this can make the language of medicine appear rather complicated for someone who speaks the language of computers, engineering, or finance. However, there are some medical conditions whose title is easily understood by both medical and non-medical folk alike because the name also describes the condition in plain English. Frozen shoulder is one of them.
What is Frozen Shoulder?
Frozen shoulder, also known as adhesive capsulitis, is a condition in which the shoulder becomes inflamed and the joint capsule itself is thickened and full of adhesions (extra connective tissue). This results in a lack of flexibility (range of motion) without a clear underlying cause such as a rotator-cuff injury or arthritis of the shoulder joint. People with this condition may one day discover they cannot comb their hair or take their shirt on and off. It may progress to a shoulder that is almost totally immobile. These can also be very painful, particularly in the early stages. It is most common in middle-aged females.
It can happen spontaneously or develop after trauma or surgery. Medical conditions like diabetes and thyroid disorders can make someone more prone to this. Unfortunately, some patients develop this debilitating problem without any warning or inciting event. Some people just wake up with it one morning!
How is it treated?
Time: Fortunately, frozen shoulder can get better on its own. However, this can take months to even a year or more and can make normal life pretty tough.
Heat: Yes, even though the shoulder is not actually cold, applying heat to the area can help increase blood flow. Doing this prior to daily stretching can help loosen the adhesions and ligaments to improve range of motion.
Physical therapy: Perhaps the most important component to ensure recovery. Too often people associate physical therapy with just getting stronger. However, physical therapists are also able to help patients regain their flexibility and range of motion through various exercises and techniques.
NSAIDs: Anti-inflammatory medications such as ibuprofen (Advil, Motrin), naproxen (Aleve), diclofenac (Voltaren gel), etc. can help calm down the inflammation and pain. However, these medications have side effects that can be harmful, particularly when used for long periods of time.
Injections: When performed by trained physicians under image guidance (ultrasound or fluoroscopy), these are very safe procedures. The purpose of these injections is to provide pain relief and decrease inflammation. Many times, steroid can achieve this purpose. However, it’s important to avoid repeat steroid injections if possible, as repeat steroid injections increase risk for developing arthritis.
PRP: Platelet-rich plasma injections (PRP), combined with numbing medicine and nerve blocks, are an excellent option. These provide up-front pain relief to assist range of motion exercises and decrease inflammation long-term using your body’s own healing chemical messengers without the side effects of steroids. PRP can be injected using precise image guidance inside the joint capsule. A fairly large volume of fluid is injected, “inflating” the joint capsule similar to a balloon. As the capsule expands, adhesive bands are stretched or released and the capsule itself is stretched. This is called “hydrodilation.” When combined with a special type of nerve block called a suprascapular nerve block to release tight muscles and reduce pain in the area, the effects can be positive and long lasting.
Manipulation: This technique is used to break up the adhesions and improve range of motion. However, this can be painful and needs to be performed either following injections or under anesthesia.
Surgery: If all else fails, surgery may become an option. This would involve surgically removing the adhesions that have formed. Unfortunately, surgery itself can result in increased scar tissue (more adhesions) and thus perpetuating the cycle.
Take Home Message:
Frozen shoulder is a relatively common orthopedic condition that can be very troublesome for patients. The tincture of time will help, but sometimes other treatments are needed in order to help the shoulder recover. It’s important that patients know their options and seek a treatment that is safe and effective.